Dinah, ClinkShrink, & Roy produce Shrink Rap: a blog by Psychiatrists for Psychiatrists, interested bystanders are also welcome. A place to talk; no one has to listen.
Thursday, June 30, 2011
Guest Blogger SG on How the Pharmaceutical Companies Have Damaged Psychiatry
Per SG:
I don't think the issue is so much a few bad shrinks but bad psychiatry. What I object to most is the pervasive compromising of science by pharmaceutical companies and all-out advertising.
This toxic influence is so pervasive that one comes to the forlorn conclusion that evidence-based medicine as it is currently practiced is really just a way for pharmaceutical companies to generate new revenue streams. The companies are so savvy they realized if they own the evidence through biased studies and suppressed trial data (failed studies, nasty side effects), they would have physicians eating out of their hands and prescribing their pills for whatever they wanted. I really think this dynamic is similar to state ownership of the media by totalitarian regimes.
Of course this is endemic in all of medicine, but psychiatry is uniquely vulnerable to this phenomenon because it has become so rigorously based on medical therapy (read: pills) since the DSM III ushered in the new "biologically based" model of mental health.
I refer the posters on this thread to the 1boring old man website in which a retired psychiatrist has been relentlessly examining internal emails between pharma execs, presentations by prominent psychiatrists like Madhukar Trivedi, seriously compromised studies like STAR-D, and various political infighting between powerful psychiatrists.
It's all very vertiginous and one comes away with the conclusion that the last 30 years of psychiatric "breakthroughs" are largely built on sand.
I think it is imperative that psychiatry look at ALL the evidence in evidence-based medicine, even if it provokes cognitive dissonance.
We must remember this about evidence-based medicine: it works on paper, but when you factor in human bias, fear, greed, and stubborn attitudes, you could have the most air-tight science (or evidence) in the world, but if it doesn't tell us what we want to hear, then the medical community automatically thinks it's flawed. How is that true evidence-based medicine?
It's time for psychiatry to come to some harsh truths and own up to them so ALL psychiatrists, even the good ones (and yes there are some good ones!) can practice at a higher standard. Even if a psychiatrist does everything right these days, I know they could do far better if they had a more honest and transparent evidence base to draw on.
Wednesday, June 29, 2011
The Chapter I Now Wish We'd Written: Bad Shrinks
I thought about this and I thought, really? We have a whole chapter called When Things Go Wrong and we discuss a psychiatrist who is not sensitive enough to a patient (though, granted, the patient is overly demanding and overly sensitive--so I guess not the best portrayal of insensitivity by a shrink), one who is rigid in her formulation to the point of almost destroying a family, one who prescribes medication that makes a patient fat and diabetic, and finally, a psychiatrist who is outright unethical and criminal: who defies all boundaries and gives her patient prescriptions for narcotics to bring back to her! Like how much worse could I make the shrinks? As one Amazon reviewer said,
The authors are careful to include what might be called opposing views. They give some space to the anti-psychiatry movement, and they consider the recent cases of medications that seem to cause suicidal thinking in some patients. But they balance that against the suicidal thinking that is prevented in some other patients by the same medications. They also talk about the influence of drug companies in a fairly open way.
There are no heroes here. The authors aren't in the business of justifying themselves, and one or two of the fictional therapists we see in the book do spectacularly bad jobs and harm patients.
But Jesse is right, overall the examples portray psychiatrists who are thoughtful and caring, and while we tried to "explain" our work, not justify it, we did not talk about psychiatrists who just plain bad, or those who are probably good but who put such an emphasis on making money that they don't give the work the time it needs.
So why didn't we (or "I," since this is my post, never discussed with my co-blogger/authors) talk about 'bad' psychiatrists in a broader way? I'm going to go for bullet points here:
- We talked about the pros and cons of split therapy, and there are pros. Clink works in a prison where she sees up to 3 patients an hour. She's a wonderful, smart, and thoughtful shrink, but I even don't believe that criminals should have psychotherapy with a psychiatrist, especially given that hard-working, insured, law-abiding people in free society can't afford this. There are all types of issues that make some rapid worse than others: if there is a single chart and the doctor has access to information from the therapist and the care is coordinated, if there are reports from other professionals treating the patient, such as in a day hospital or program setting, where assessment includes a team approach, medications can be managed well with less face-time with the patient. In a private practice setting, however, rapid care may mean shoddy care.
- At the time we wrote the book, I had never heard of an outpatient, private practice, psychiatrist who sees 40 patients a day such as the one portrayed in the NYTimes article by Gardiner Harris. I'd heard of 15 minute med checks, but in the clinic where I work, I sometimes see patients for 15 minutes, or less, not because I'm scheduled so tightly, but because they have nothing to say...all is well, a family member is there and confirms that things are going smoothly, their therapist is in the room and says things are fine, and the patient wants their prescription refilled and to get out. I had never heard of an outpatient psychiatrist who sees every patient, regardless of their needs, in a one-size-fits-all 15 minute slot. I can't imagine how this can be done well. The New York Times may want to portray this as how psychiatry is now routinely done, but it's not.
- Some psychiatrists are insensitive... we did reference the idea of a psychiatrist "with the social skills of an iguana" (I hope we didn't insult any iguanas!), but the idea of interpersonal sensitivity is a hard one to capture--- people are very different in what they want, and one person can relay a story with "Can you believe he said THAT?" While another person would find THAT as being a perfectly reasonable thing to say. There is no psychiatrist out there who is everyone's perfect fit, and even the people I might think I'd never refer to, likely have devoted patients with good outcomes.
- The things that often trouble patients the most are endemic to all fields of medicine these days and not just psychiatry and they don't objectively make a doctor "bad," (maybe over-scheduled, disorganized, or forgetful) and include the large areas of running late and keeping patients waiting, or of not returning phone calls. Patients are often angry about this---often rightfully so--because it leaves people feeling like they aren't cared for or respected. I'm not certain what there is to do about this one.
Sunday, June 26, 2011
Understanding the Research on Psychotherapy Trends-- a Discussion with Dr. Ramin Mojtabai
For whatever reason, it bothers me when media says that psychiatrists don't do psychotherapy, and lately, it happens a lot. What am I, chopped liver?
They quote a study by Mojtabai and Olfson in the Archives of General Psychiatry, and say, "Only 10.8% of psychiatrists see all of their patients for psychotherapy." Is that really true? Is it really relevant? I tried to read the article and I wanted to understand how the study was done so I could think about it myself, but I didn't understand how the research was done-- Roy thought it was based on CPT codes, then he said it wasn't. So why not go to the source? I asked Dr. Mojtabai if he would have lunch with me and tell me how the study was conducted.
If that got you curious, please read about it on over on Shrink Rap News! You're welcome to comment there if you're physician, or to surf back here and tell us what you think. Ramin says he's interested in what people think, and he's been very kind about humoring me, both over lunch and in the many subsequent emails over the details.
Saturday, June 25, 2011
The Ten Percent Solution
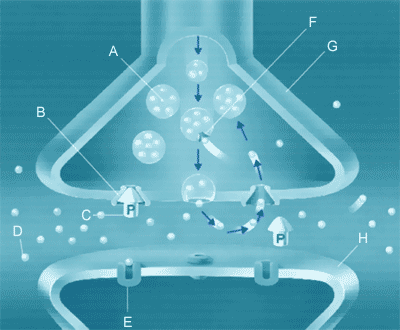
In response to a change in the brain's biophysicochemical stew (meds, trauma, chronic stress, etc), it generally takes neurons a couple weeks to fully generate new or recycle old protein machinery -- to adapt to changes. This duration can be shorter for some proteins, longer for others. Thus, small changes would be expected to minimize the shock to the system. This just makes good homeostatic sense.
There are problems with this as dogma, however. There is not useful research, at least that I am currently aware of, to demonstrate whether the "best" interval percentage change is 10% or 5% or 25%. We also don't know if the "best" interval is one week, two, four or eight. Or which medications and their affected pathways are best tapered at what intervals and amounts. Please share original source (ie, PubMed) links to peer-reviewed research below if you have relevant references.
Quacks....
 | |
| From Broom Hilda |
I'm wondering what she wanted validated? Her parking ticket, perhaps?
Friday, June 24, 2011
Guest Blogger Dr. Jesse Hellman: Tarzan, the Computer, and the Unconscious
Psych Meds are THE Problem: A Post for Duane Sherry
I see patients who walk in the door in distress. The only people who walk in feeling well are those who have been treated by someone else and are coming to continue treatment, either because their shrink moved, they moved, something changed.
Once in a while, someone comes in and they are in distress and they are already on psych meds and I look at the regimen and say "No wonder you feel badly, you're on way too much medicine" and I stop things. Mostly though, I start new medicines and I see people who were sick get better. Some people have problems with medicines, but not like I hear people talk about in our comments section. Here at Shrink Rap, people hate anti-psychotics. Very few patients tell me that very low dose anti-psychotics bother them. Medicines need to be added carefully, at low doses, and increased gradually. The patient is supposed to get better: it they don't, the medicine should be stopped. Sometimes people end up on a zillion medications, no better, and it's not clear why they are on them. See: Medications: The Good, Bad & Ugly, and You're Supposed to Get Better. These are some of my views on treatment and medications.
It's not unusual that patients come in and casually mention in the course of a therapy session, "oh, I stopped taking the meds." I ask why. Side effects? Felt they were no longer necessary? I ask if they feel better without them (some do, some don't). I'm here to help, and since I work in a totally voluntary setting, I may spout statistics, especially to someone with a high risk of relapse who was having no side effects and no problems with the meds and feels no differently off them-- but hey, you don't want to take medicines-- it's fine with me, and I'll hang out with you in therapy anyway.
Duane Sherry has been visiting us for a while now in the comment sections and he feels strongly that medications are the problem, not the answer, and that people who think they are better are wrong. He and I are seeing different before & after shots. He asks if I give informed consent (funny, I do) and thinks people should explore different options such as orthomolecular therapies. He's posted many links, and something gets troubling about the repetitive nature of it (at least to me) and something gets troubling about the accusatory tone, though he has really toned down the blatant --you're an idiot-- comments. Thank you, Duane, this has meant a lot to me.
So let me give Duane a moment here to get out his message of Meds are Harmful / Psychiatry Sucks here on the main page of Shrink Rap. Duane, you're still welcome to comment, but please stop with the repetitive links, and please keep the tone respectful. You might want to consider getting your own blog where like minded people can have a forum.
Duane says:
They provide temporary relief.
And that's all they do.
The greatest injury happens in their long-term use... They are addictive, because they meet the medical definition of physiological addiction in two vital areas:
a) Increased tolerance
b) Measurable effects during withdrawal
Have your patients look at the "side effects" more closely... Really look at what the drugs do.
Then see how many want to be placed on them.
Here is Duane's website...funny, no place for comments:
http://discoverandrecover.wordpress.com/wellness
Here are some links Duane likes:
http://www.foodforthebrain.org/content.asp?id_Content=1635
http://www.vitamindcouncil.org/health-conditions/mental-health-and-learning-disorders/depression/
http://www.townsendletter.com/Nov2009/hoffer1109.html
http://www.youtube.com/watch?v=aBjIvnRFja4&feature=channel_video_title
http://www.madinamerica.com/madinamerica.com/Timeline.html
http://breggin.com/index.php?option=com_content&task=view&id=40&Itemid=52
http://recoveryfromschizophrenia.org/therapists-guide-to-reducing-medications/
Duane, Please put any other links you'd like in the comment section of this post: your personal space on Shrink Rap. If you'd like, in future comments you can say "I'm putting links up in my space on Shrink Rap" and link back to this post and put them in the comment section here.
For the most part, we need to agree to disagree. I don't believe I am going to sell Duane on the idea that medications sometimes help people live better lives. And I don't think he's going to sell me on the idea that they should never be used.
To my co-bloggers: please forgive me.
Thursday, June 23, 2011
Article on Marsha Linehan in Today's NY Times
And Please Visit Clink's post over on our Shrink Rap News blog on ethical issues related to the psychological report on the suspected Anthrax killer.
When you're finished reading, please return Here to comment.
Marsha Linehan arrived at the Institute of Living on March 9, 1961, at age 17, and quickly became the sole occupant of the seclusion room on the unit known as Thompson Two, for the most severely ill patients. The staff saw no alternative: The girl attacked herself habitually, burning her wrists with cigarettes, slashing her arms, her legs, her midsection, using any sharp object she could get her hands on.
The seclusion room, a small cell with a bed, a chair and a tiny, barred window, had no such weapon. Yet her urge to die only deepened. So she did the only thing that made any sense to her at the time: banged her head against the wall and, later, the floor. Hard.
“My whole experience of these episodes was that someone else was doing it; it was like ‘I know this is coming, I’m out of control, somebody help me; where are you, God?’ ” she said. “I felt totally empty, like the Tin Man; I had no way to communicate what was going on, no way to understand it.”
This is a great article, check it out. Thanks, Jesse, for the heads up, and Rob, for the link.
Wednesday, June 22, 2011
Suicide, Free Will, and the Shrink's Magical Ability to Predict Violence
I'm posting over my fellow co-bloggers today. So what else is new?
When you're finished reading, please return Here to comment.
CPN: The Anthrax Report
In ClinkShrink's post on Clinical Psychiatry News she points to some ethically troubling actions in the official investigation into Dr. Bruce Ivins's alleged involvement in the 2001 Anthrax attacks, including the sale of a report containing his medical records.
Tuesday, June 21, 2011
Summer Solstice: "Hot" Grand Rounds on Shrink Rap
We received
The signs of heat exhaustion often begin suddenly. Symptoms resemble those of shock and may include feeling faint or dizzy; nausea or vomiting; heavy sweating; paleness; muscle cramps; weakness or tiredness; and headache. The skin may be cool and moist. The pulse rate will be fast and weak, and breathing will be fast and shallow. Untreated, heat may progress to heat stroke.
In addition to the new labeling, the FDA has proposed to limit the maximum SPF value on sunscreen labels to "50+", because there isn't enough evidence to show that products with higher values provide any more protection. FDA is now seeking public input on that. The FDA is also reexamining the safety information available for active ingredients included in sunscreens marketed today.
In A Medical Resident's Journey, Another Day, Another Summer... reflects on the different sorts of summer maladies appearing in the summer Emergency Department.
Heat rises from the sidewalks of the city. Backyard grills appear again. Sun dresses, outside tables, kites, picnic baskets, bike riding. The world welcomes us to summer. In the hospital, it is a time of great change. All of us – residents, fellows, medical students – are moving on in our journey. Over a period of a few weeks, we will be “promoted” to new positions in the hospital. Some of us – those who have completed their training – will be leaving, to become attending physicians at last.
Dr Nicholas Fogelson from Academic OB-GYN sent in One for the Medical Students -- on Presenting, explaining how med students can give HOT patient presentations. Okay, that was a big stretch, as we couldn't determine any link here to the summer solstice nor summer pictures. Wait, I've got it... at the end of each patient discussion, one should provide a very Summery presentation!
A student that never jettisons the note cards will never be an effective presenter.
David Williams from Health Business Blog gave us some HOT hospital clowns in action in Hospital Clowning: Video Introduction to Hearts & Noses Hospital Clown Troupe.
The clown aspect people think they get, but it’s hard to explain how empowering the professionally trained, dedicated volunteers are to the thousands of children and families they serve.
Brooke Douglas from DrPullen decided to inflame us with Inflammation and Diet: Inflammatory and Anti-Inflammatory Foods.
Hot stuff!
The problem occurs when chronic inflammation occurs inside our body and we can’t see it or feel it. This chronic inflammation does not allow for natural repair and healing caused by the damaging ‘pro-inflammatory’ (saturated and trans) fats.
Bob Vineyard from Insure Blog sent in Georgia Piedmont Hospital Layoffs. In a move that's sure to leave docs and patients hot under the collar, an Atlanta hospital is laying off over 400 health care workers.
Georgia, looking for new revenue, decided the prudent thing was to implement a hospital bed tax. As with any other tax imposed on business, the customers (patients) pay the tax. The irony is, the bed tax was introduced to make up for current budget problems in funding Medicaid. It makes you wonder what will happen when Obamacrap expands the Medicaid rolls in 2014.

Zoe Brain sent in a post from Box Turtle Bulletin, which features "news, analysis and fact-checking of anti-gay rhetoric." She describes the post, What Are Little Boys Made Of?, written by editor, Jim Burroway, as HOT as in timely, radioactive, controversial. It is a stirring description of past "treatments" for homosexuality during a period when even having effeminate traits was considered a sign of disease. The long-term consequences to Kirk "Kraig" Murphy, a 5-year old in 1970 and the subject of a series of research papers, are chronicled here.
In this original BTB investigation, we speak with [Kirk's] family and friend who knew the real “Kraig” to uncover the truth behind [researcher] Reker’s greatest success story. Their stories reveals the tragedy of a terrible experiment on a very young boy which would haunt him for the rest of his life. It is not only an indictment of a man who built his anti-gay career on Kirk’s suffering, but a rebuke to others — those in the mental health profession then and in the contemporary ex-gay movement today — who would place their careers and agendas ahead of the well-being of this young boy and countless others like him.
Louise Norris from Colorado Health Insurance Insider sent in her HOT topic: Rate Review Process Does Not Keep Insurance Premiums Artificially Low. Last year or so, framing the whole health care reform discussion, a large California insurer announced 39% rate hikes. This post discusses a California bill that would require rate regulation by the state's insurance commissioner, which many states currently have, and a research article finding that rate regulation does not put insurers out of business.
Having rates approved by the DOI does not mean that the people of Colorado get smaller-than-average premium increases. Rather, it means that although our rate increases are sometimes substantial, we know that those rates are justified as a reflection of increasing claims costs.
South African surgeon, Bongi, blogs on Other Things Amanzi. He sent in Dolls Eyes, about his experience as a fourth-year medical student helping a woman with a tragic fetal loss.
i remember sitting there in that small labour room where mothers are usually introduced to their new babies while the registrar ran the sonar probe over the mother's swollen abdomen. i remember her bringing the probe to a standstill over the heart. we could clearly see the heart, but there was no movement. the heart was not beating. as we actually already knew, the baby was dead. all that remained was to tell the mother.
Erin Breedlove, who has cerebral palsy, submitted a post from her blog, Healthy, Unwealthy, and Becoming Wise, about what to say to children when they ask her, What's Wrong With You?
To me, it’s a pretty poignant, honest question because there are some days that I’m not sure how I’d answer it to anyone, much less myself. As a future educational psychologist, I’m a fierce advocate for giving children all the information. No, they might not be able to understand the full extent of what you mean at their current age and stage of development, but trust me, they’ll appreciate it later... One of the most common questions I’m asked is about why I don’t use the “everybody’s different” response, and there are two reasons in addition to the ones outlined above. The first is that I believe that the response undermines the intelligence of a child, and that’s the last thing anyone wants to do during critical stages of development, and the second is that I believe that the only way children will learn and understand is to be inquisitive, so I appreciate that with everything in me.
Jacqueline from Laika's MedLibLog gives us the low-down on the question of Does Soy Relieve HOT Flashes?
The other phytoestrogen interventions were very heterogeneous with respect to dose, composition and type. This was especially true for the dietary soy treatment. Although some of the trials showed a positive effect of phytoestrogens on hot flashes and night sweats, overall, phytoestrogens were no better than the comparisons. Most trials were small, of short duration and/or of poor quality... One striking finding was that there was a strong placebo effect in most trials with a reduction in frequency of hot flashes ranging from 1% to 59%.
The med student at Metropolis Med posted on Action Potential about 5 Memorable Moments as a first-year medical student where she lost her cool (losing cool = HOT!).
2. That time the med school dorm decided to test every smoke alarm.
3. That time we were assigned 250 pages of reading in one day.
Sarebear posted on Across and Inside My Universe about those times When the Doctor/Patient Relationship Becomes Heated.
Before I get into specifics, let me say that as a patient, when you are sitting there on the receiving end of some "heat", or ire, or intense aggravation, or anger, even, it is shocking, bewildering, and causes you to wonder what is wrong with you or what you did wrong, as the patient, to deserve what is happening. You are shocked because, if you've had enough dealings with this doctor (about a year, in my first psychiatrist's case, when this happened) you know that he normally conducts himself much more professionally; to see and FEEL such unfettered, intense, unpleasant emotion, directed at YOU . . . well to say it is bothersome is an understatement.
Rachael Watman from the John A Hartford Foundation blog wrote about the HOT topic of Helping Hoarders, profiling the work of Monika Eckfield RN PhD.
I interviewed 22 adults age 65 and older, six men and 16 women. My oldest participant was 91. Most of them lived alone. Most had hoarding behaviors to varying degrees all their lives. When you’re living with someone there tend to be checks and balances, and the home doesn’t get overwhelmingly cluttered. When a person gets divorced or becomes widowed they no longer have the checks and balances. Other life changes can also exacerbate hoarding behavior...
Julie Rosen of Bedside Manner, from the Schwartz Center for Compassionate Healthcare, wrote about the passion behind Massachusetts First Lady Diane Patrick and her experience of Compassion for the Mentally Ill. [submitted by Petra Langer]
Today, Mrs. Patrick’s advice to those suffering from depression is to seek help and to be open to compassion. “Because I admitted my problem, I allowed compassion to come to me,” she says. “Not only did I receive compassionate care from my wonderful therapist, I was treated with compassion by those around me – and the abundance of compassion I received helped me to recover.”
Kimberly Grady wrote Life at Grady: Stop, Look, Listen, posted on ACP Hospitalist. The patient presents with a fever and leg pain after a bad pedicure.
I immediately covered my mouth, forgetting that I was in earshot of my attending. Then I said it again as I skimmed the abstract of that article. The second time, I didn't even bother covering my mouth. This "damn" wasn't a "Damn, I should've known that!" It was a "Damn, this dude knew what was wrong with this patient just from the bedside." Or better yet "Damn, when I grow up, I'm TOTALLY going to roll up on a patient's bedside and nail a diagnosis just like that."
Ramona Bates from Suture for a Living tweeted her submission about The Impact of Obesity on Breast Surgery Complications, which she swears is a HOT topic in her field.
Overall, 18.3% of obese patients had a complication compared to only 2.2% in the control group (p<0.001). After adjusting for other variables, the researchers found obesity status increased the odds of experiencing a complication by 11.8 times.
Elaine Schattner from Medical Lessons emailed a related HOT topic from Wired, Human Milk for Sale, Where's the FDA?
As much as I think it’s a good idea for women to breast feed their babies as best they can, I was pretty shocked to learn about this unregulated industry. Mainly because if a woman who donates milk is infected with a virus, like HIV or HTLV-1, the milk often contains the virus. The infant can absorb the virus and become infected. Feeding human breast milk from an unknown donor is kind of like giving a child a blood transfusion from a stranger, unchecked by any blood bank.
Glenn Laffel from Pizaazz emailed The Effectiveness of Online Health Intervention Programs, talking about the HOT new trend of medical apps, particularly the online videogame, Re-Mission.
Re-Mission is intended improve medication compliance in teens and young adults with a history of cancer. In the game, players control a nanobot within a 3-dimensional body of a young person that has cancer. Play involves destroying cancer cells and managing chemotherapy-related adverse effects like vomiting and bacterial infections by using antiemetics and antibiotics. The game purports to help users understand their disease and its treatment and improve their sense of self-efficacy: they can take control of their disease.
And the
I was impressed. This is what every pharmacy should be like – except, of course, for the dinginess, the creeping line and the fact that it was so crowded I could overhear these conversations. Maybe if we got federal legislation enacted requiring pharmacists to offer counseling with each prescription filled, this kind of attention would be the norm, adherence to medication regimens would improve and drug-related injuries would be reduced. Wait a minute. Someone already had that good idea.[these last three posts were accidentally left out of the initial draft... sorry guys]
The Happy Hospitalist was thinking about how to explain those unwritten Bathroom Etiquette and Rules for Public Restroom to his young son [get it?].
- Always leave at least one urinal between you and another person
- Do not look at others while urinating
- No touching
Beth Gainer in Calling the Shots is a little steamed about the unintended fall-out from a National Cancer Survivors Day.
Just when the marketing of cancer feel-good gimmicks cannot get more insulting, there's National Cancer Survivors Day. Oops, I forgot to include that pesky little registered symbol.
Romeo Vitelli in Providentia sent in a radioactively hot post on the history of radium in That Healthy Glow.
By 1917, the United States Radium Corporation had patented the first glow-in-the-dark radium-based paint (with the brand name of Undark). Between 1917 and 1926, the company employed hundreds of female workers to paint luminous watch dials under uncontrolled conditions. The workers (later known as the Radium girls) had been reassured that radium-based paint was harmless and no industrial safeguards were in place to limit contamination. ... the factory managers encouraged the workers to use their lips and tongues to wipe off the paint. Some of the workers even went to far as to use Undark to paint their fingernails as an odd fashion statement. By the time the toxic consequences of radium exposure became apparent, it was far too late for them.
 Okay, so that's the end of our Hot Grand Rounds. Do have a safe and healthy summer! Be sure to check out next week's Grand Rounds host, Colorado Health Insurance Insider.
Okay, so that's the end of our Hot Grand Rounds. Do have a safe and healthy summer! Be sure to check out next week's Grand Rounds host, Colorado Health Insurance Insider.=Steve Daviss MD, co-author of Shrink Rap: Three Psychiatrists Explain Their Work.
Sunday, June 19, 2011
Please Complain
For those who don't follow the comment sections of posts, there have been commenters who have been telling us about the awful experiences they have had as psychiatric patients. In particular (but not exclusively) as hospital inpatients. Commenters have used terms like "abuse" and "humiliation" and describe awful scenarios. One person asked why the mean nurses don't get fired, everyone knows they are mean including the staff. Others throw the baby out with the bath water, one bad experience. There is implication by at least one commenter that he/she would rather die (presumably permanently) rather than face a days on a psych unit again. The suffering in these posts is palpable.
To those who feel better after leaving comments on Shrink Rap, by all means, feel free to continue, but this will not change the world. May I put in a request? If you've had an awful experience as a patient on a psychiatric unit, please tell the hospital. One commenter said she (/he?) complained to the hospital administration and heard that some changes were made. My thoughts? You Go Girl! (If the commenter was a male, I'm at a loss. Way to Go, Joe! perhaps?) Complain, it can't hurt.
Oh, you say, no one listens to psychiatric patients, they just say we're crazy so they don't have to listen. For an isolated complaint, you may be right, especially if the complaint is about something that is not egregious. But if everyone who feels wronged complains, then it won't be an isolated complaint, and I can tell you that for administrators, one person accusing is a fluke --or a psychiatric patient they don't need to listen to-- but at a very low threshold of two or three complaints, it quickly becomes "PEOPLE are complaining about such and such" and someone starts to notice. If the complaint is egregious (My nurse punched me) then a single complaint should have an impact.
Who should complain? If you were upset over something that happened and it continues to linger, you can't let it go, and you continue to feel angry, wronged, and injured, then you should complain.
So let me tell you how to complain.
1). Call the hospital and ask where to direct a complaint and get a person's name and postal or email address. Also send the same letter to the chairman of psychiatry, and the head of the hospital...why not? Address the letters to specific people by name; "Dear Sir," "To Whom It May Concern," or "To the Sadist Creep on the Psych Unit" will not go far.
2). Just the facts, ma'am. Tell the administrators when you were hospitalized and that you continue to feel distress/angst/anger/whatever you feel about things that happened while you were in the hospital and give a bullet point list of the things that continue to trouble you. Include specific examples, if you can, names of those who were involved. If you don't recall specific examples, it still seems to me it's valid to say "Shrink John treated me in a harsh and disrespectful manner." Say how you felt: "It was humiliating to be stripped and placed in a seclusion room."
3). This is not the time for name-calling, hater rants, or discussing the care of other patients. "This is why everyone hates psychiatrists," "You people over-medicate everyone," Pretty much guarantees that the recipients shut down. Stick to your problem. Be polite and respectful and try not to compare the mental health professionals who treated you to serial killers.
4) Sign your name and leave contact information.
5) Show it to a friend first and wait a day to send it.
I don't know if you'll get a response or a change, but if everyone who feels as wronged as our commenters do writes to complain, then things will change. It may take time. Don't be hater, be a changer.
Thank you for considering my suggestion.
Happy Father's Day to all, and remember to submit your Grand Rounds post now.
Saturday, June 18, 2011
The Top Ten or More Things That Annoy Me About Psychiatry Haters
9. Insults directed by psychiatry haters at the Shrink Rap bloggers. Disagreement is one thing, insults are another.
8. Insults directed at other commenters on Shrink Rap.
7. The implication that all (or even the majority) of psychiatrists are purposefully evil and have mean intentions when treatment has bad outcomes. Most of us don't have personal relationships with the devil. At least I don't think so.
5.5 The implication that psychiatrists uniformly push medications on unwilling patients. In the outpatient setting, patients often come requesting medications, or requesting to continue medications that they have found to be helpful.
5. Statements that someone was perfectly fine until they took psychotropic medications. People generally seek psychiatric care and medications because something is wrong. This is not to say that medications don't have side effects that might be worse than the problem they were treating.
4. Statements that psychiatrists personally benefit by keeping patients in the hospital and "incarcerating" people who are well for prolonged periods of time. Psychiatrists are under tremendous pressure to keep lengths of stay as short as possible, they have to personally call and argue with insurance companies to justify each day of inpatient care--this is not fun.
3. Statements that psychiatry "incarcerates" people without due process. There is due process, but it takes time, and it is true that someone can be kept on a hospital unit for days until 1) the psychiatrist is able to make a reasonable evaluation and 2) the legal system is put in motion-- most hospitals have a specific day of the week where a judge comes to hear both sides. In any system that employs due process, there is the possibility of miscommunication, misinformation, misunderstanding, lying, or mistakes.
2. The implication that the average practicing psychiatrist had some way of personally knowing that Big Pharma manipulated research and withheld side effects and adverse effects of medications and they should have not prescribed those medications.
1.5. Sensationalism by the media on the all of the above in an unbalanced way. For example, there was a recent news story about how atypical anti-psychotic medications are prescribed for agitation to patients with dementia when they do not have a FDA approval for this indication. The article did not mention that there is no medication that has FDA approval for agitation in dementia. The article also does not give any examples of things such as patients who are miserable in their agitation, who strike their caregivers, who repeatedly end up injuring themselves. (This isn't to say that I believe that it is always appropriate to give patients with dementia antipsychotic medications, or that giving these patients a better environment or improved care wouldn't allow them to manage without them, it's simply to say that I would want journalists to present a balanced view with a number of scenarios).
1.25 Implications that psychiatry as a field is inflexible, finds itself above reproach and is unwilling to listen to criticism. We still have a long way to go to reach perfection, but every year things change: we've come a long way from the days when someone could be committed to a hospital for years for trivial reasons, we look at treatment more as a partnership, and we have more (albeit imperfect) treatments to offer. There are too many ways to list how care has changed over the last 50 years. My gripe is not with criticism or with a desire to change the way things are done, it's with a particular form of delivery of the message.
And the number one thing that psychiatry haters say that annoys me:
1. The implied statement, "This psychiatric medication harmed me so it should be illegal for anyone else to take any psychiatric medication." It's disrespectful to those who find medications to be beneficial.
To read many of the comments on our Shrink Rap posts, one might think the psychiatrist-patient relationship is an adversarial one. I just haven't found that to be true.
Comment away, and please don't forget to submit your Grand Rounds posts by Sunday night!
Friday, June 17, 2011
Budgets, Crime and What Happened to Stephanie
 From the New York Times today we have a story entitled, "A Schizophrenic, A Slain Worker, Troubling Questions," a horrible story about a mentally ill man who killed a social worker in his group home. The story highlights the defendant's longstanding history of violence with several assaults in his past. He once fractured his stepfather's skull and his first criminal offense involved slashing and robbing a homeless man. (On another post on this blog Rob wondered why the charges were dismissed in that case; from experience I can tell you it's probably because the victim and only witness was homeless and couldn't be located several months later when the defendant came to trial.) The defendant, Deshawn Chappell, also used drugs while suffering from schizophrenia. Before the murder he reportedly stopped taking his depot neuroleptic and was symptomatic. The news story also suggested that he knew he was committing a crime: he got rid of the body, disposed of the car and changed out of his bloody clothes. Nevertheless, he was sufficiently symptomatic to be found incompetent to stand trial and was committed to a forensic hospital for treatment and restoration. At his competency hearing the victim's family thought that the defendant was malingering his symptoms, while the victim's fiance was distraught enough that he tried to attack Chappell in the courtroom. The point of the Times article appears to be an effort to link the crime to cuts in the Massachusetts mental health budget.
From the New York Times today we have a story entitled, "A Schizophrenic, A Slain Worker, Troubling Questions," a horrible story about a mentally ill man who killed a social worker in his group home. The story highlights the defendant's longstanding history of violence with several assaults in his past. He once fractured his stepfather's skull and his first criminal offense involved slashing and robbing a homeless man. (On another post on this blog Rob wondered why the charges were dismissed in that case; from experience I can tell you it's probably because the victim and only witness was homeless and couldn't be located several months later when the defendant came to trial.) The defendant, Deshawn Chappell, also used drugs while suffering from schizophrenia. Before the murder he reportedly stopped taking his depot neuroleptic and was symptomatic. The news story also suggested that he knew he was committing a crime: he got rid of the body, disposed of the car and changed out of his bloody clothes. Nevertheless, he was sufficiently symptomatic to be found incompetent to stand trial and was committed to a forensic hospital for treatment and restoration. At his competency hearing the victim's family thought that the defendant was malingering his symptoms, while the victim's fiance was distraught enough that he tried to attack Chappell in the courtroom. The point of the Times article appears to be an effort to link the crime to cuts in the Massachusetts mental health budget.
So what do I think about this story? (As Dinah would say, this is a 'Clink' thing.)
About the crime itself I have little to say. There's nothing that out-of-the-ordinary or unusual about this as a forensic case. I have no opinion about his legal sanity since I know nothing other than what's presented in the media (and I've had enough of my own cases covered in the media myself to take what I read with a large grain of salt!). Frankly, these kind of cases happen every day as you could tell by following the Psychiatry and the Law twitter feed.
Why does this story, of all the potential psychotic killer stories, showing up in the New York Times, and why is it showing up now?
Because New York is trying to "beef up" their assisted outpatient treatment law, of course. And the Times has come out in favor of it. They've had other articles in the paper promoting assisted outpatient treatment.
Now, I'm all in favor of advocating for improved mental health services as well as adequate training and reimbursement for well-qualified mental health staff. I just wish they wouldn't feed into the fear and public stereotyping of seriously mentally ill people to do it. That's my first reaction to this piece.
My second reaction is in response to this quote:
"The first time Mr. Chappell secured a state hospital bed — and the treatment that comes with it — was when he ended up behind bars."And the observation by Chappell's mother:
"In 2007, Mr. Chappell, sentenced to a year in jail but required to serve only three months, ended up at the prison psychiatric hospital. When his mother visited him there, she said, she was heartened to see the effects of an enforced medication regimen. “This was the son I raised,” she said. “He talked about going back to school and getting a college degree.”I'm going to link back to those quotes the next time I hear somebody comment that "locking people up doesn't do any good." There are some people---fortunately relatively few---who can only be treated in a secure environment because they are just too repetitively assaultive to be treated anywhere else. That's what forensic hospitals and prisons are for.